|
12/11/2023 0 Comments Axillary sentinel lymph node biopsy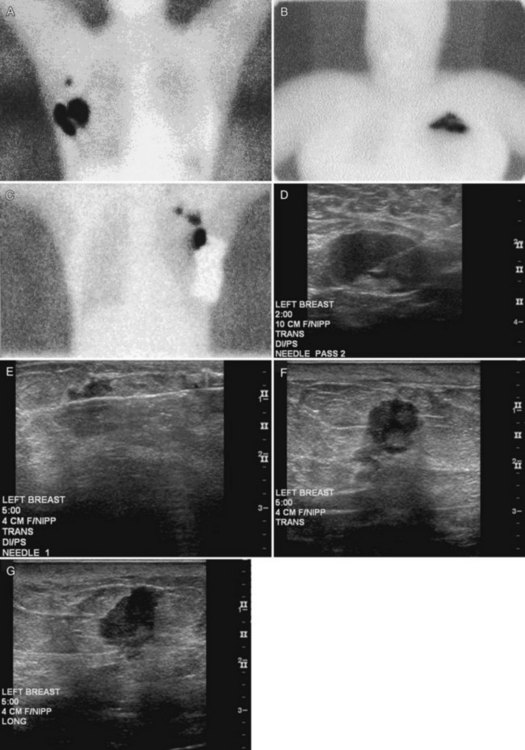
The concept of sentinel lymph node surgery is to determine if the cancer has spread to the very first draining lymph node (called the "sentinel lymph node") or not. In these cases, if the cancer spreads it will spread first to lymph nodes (lymph glands) close to the tumor before it spreads to other parts of the body. The spread of some forms of cancer usually follows an orderly progression, spreading first to regional lymph nodes, then the next echelon of lymph nodes, and so on, since the flow of lymph is directional, meaning that some cancers spread in a predictable fashion from where the cancer started. The sentinel node procedure (also termed sentinel lymph node biopsy or SLNB) is the identification, removal and analysis of the sentinel lymph nodes of a particular tumour. In case of established cancerous dissemination it is postulated that the sentinel lymph nodes are the target organs primarily reached by metastasizing cancer cells from the tumor. The sentinel lymph node is the hypothetical first lymph node or group of nodes draining a cancer. The axillary lymph nodes drain 75% of the lymph from the breasts((uncited)) and so may be the first lymph nodes affected in breast cancer. The surgeon may use a combination of the gamma probe and a blue dye to find and surgically remove the lymph node.First lymph node to receive drainage from a primary tumor Image illustrating sentinel lymph nodes. If anterior hip supports are in place, ensure they are properly padded or neuropraxias and/or occlusions of large blood vessels may result. Pad all dependent bony prominences such as the fibular head (to prevent peroneal nerve injury), and place pillows between the knees and ankles (to prevent saphenous nerve injury). If a bean bag is employed, check the hard edges to ensure that unnecessary pressure isn’t being put on soft tissues. If the non-dependent arm is placed on a board, check padding and reposition regularly to avoid radial nerve compression. Check routinely to make sure the axillary roll does not migrate into the axilla. To prevent this, place an axillary roll under the patient (caudad to the axilla, on the rib cage, and NOT in the axilla). These are motor and/or sensory loss for 6-8 weeks due to pressure on the contralateral (dependent) axilla. The most common nerve injury for orthopedic lateral procedures are neurapraxias of the brachial plexus. Once lateral, use pillows/blankets/foam headrest to keep the patient’s head in neutral position. Unhook anesthesia circuit while turning lateral and be especially careful to keep patient’s head neutral and aligned with body to avoid neck injury. Lateral position (general considerations): If an ETT has been placed, make sure ETT is secure with extra tape. Keep your connections and tubing where you’ll have fast access. Positioning of the leads is typically high on the posterior and posterolateral back (somewhere free of pressure and out of surgical borders). Check the patients eyes/ears/nose regularly throughout the case to ensure they are free of pressure. Eye protection should be used as the prone position heightens the risk of corneal abrasion and/or traction on the globe (which can result in blindness). The patients arms are typically flexed, which will kink the IV. Prone Position (general considerations): Maintain cervical neutrality. Be cautious of having the patient too light as this will be especially stimulating. Typical positioning – The surgeon typically likes the affected side rotated up towards him/her along with reverse trendelenburg.Įnd of case – The patient may be hand-hoisted to the sitting position at the end of the case to allow application of a chest binder or wrap. Surgeons like the twitch as an indicator that they are close to the nerve. Use of cautery in the affected area will cause a twitch when getting close to these nerves. This is because he/she will be working close to the thoracodorsal and/or long thoracic nerve. Succinylcholine is fine to get the case started, but the surgeon will need the patient to be paralytic-free later in the case. Non-depolarizing muscle relaxants – Intentionally AVOID long-acting muscle relaxants/paralytics. Most often, the biopsy will be done by a general anesthetic approach.īelow are the indications for breast cancer (one of the most common) So, the anesthetic approach and position here really depends on the location of the cancer. Position: Supine, Reverse Trendelenburg, Prone, Left Lateral, Right LateralĪ sentinel lymph node is the first lymph node a malignant cancer is likely to spread to.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
